Bariatric surgery assists you in losing weight and can lower any risk of medical issues that come from obesity. How does weight loss surgery help you lose weight? There are two significant reasons weight loss surgery helps.
Restriction. Having weight loss surgery will physically limit how much food you intake. Your stomach will not be able to hold as much food which means you will eat fewer calories.
Ghrelin. The hunger hormone, ghrelin, is reduced. You won’t feel hungry throughout the day.
Four common types of weight-loss surgery are:
- Sleeve gastrectomy, also called gastric sleeve
- Roux-en-Y, also called gastric bypass
- Laparoscopic, also called adjustable gastric banding
- Duodenal switch

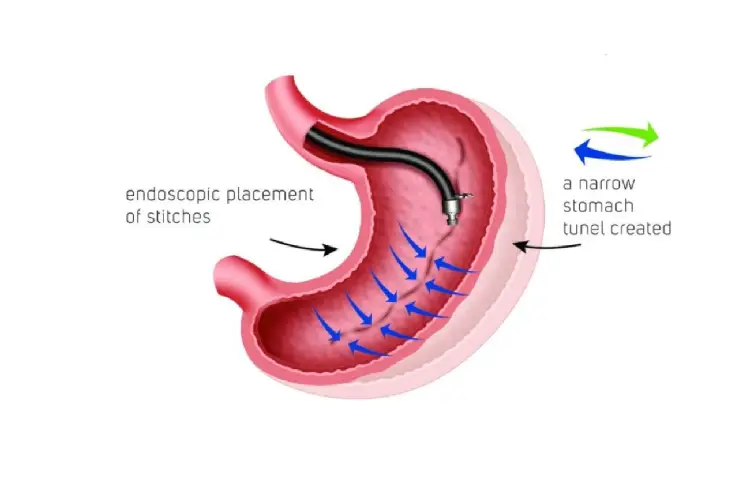
Sleeve gastrectomy
With gastric sleeve surgery, a portion of the stomach is removed from the body. The part of the stomach that remains in the body is formed into a tubelike shape. After gastric sleeve surgery, you will produce less of the appetite-regulating hormone ghrelin, this will lessen your desire to want to eat. What makes the gastric sleeve surgery different than some of the other surgery types is that the sleeve gastrectomy does not affect the absorption of calories and nutrients in the intestines.
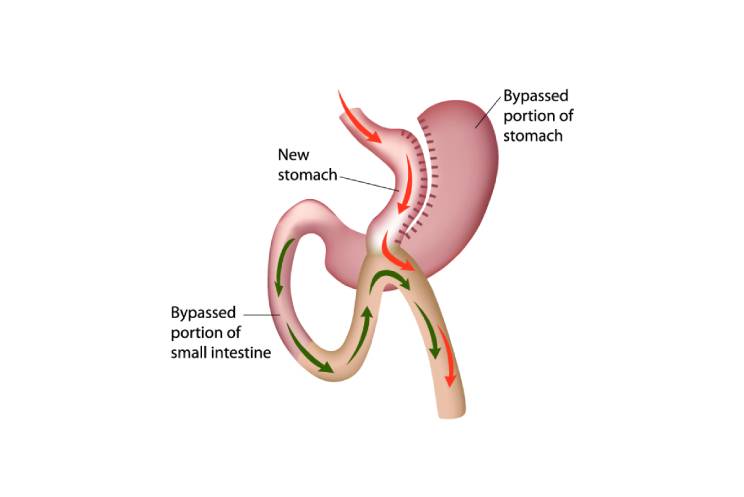
Roux-en-Y gastric bypass
With gastric bypass, a small pouch is created at the top of the stomach. The small pouch is the only part of the stomach that will receive food. This limits the amount of food you will eat or drink at one time. Just below the main stomach, the small intestine is cut and connected to the new pouch. Food will flow directly from the pouch into this part of the intestine. The main part of the stomach will continue to make digestive juices. The part of the small intestine that is still attached to the main part of the stomach is reattached further down. This helps the digestive juices to flow through to the small intestine. Food will now bypass a portion of the small intestine allowing fewer nutrients and calories to be absorbed.
Laparoscopic adjustable gastric banding
With adjustable gastric banding, a band that houses an inflatable balloon will be placed around the upper part of the stomach and will be fixed in place. This will create a smaller stomach pouch right above the band with a very small opening to the rest of the stomach. A small port is then placed just below the skin of the abdomen with a tube connecting the port to the gastric band.
To adjust the size of the band, fluid will be injected or removed through the port. Gastric banding restricts the amount of food that your stomach can hold. You will feel fuller sooner. Gastric banding doesn’t reduce the absorption of calories and nutrients.
Biliopancreatic diversion with duodenal switch
Similar to gastric sleeve surgery, the duodenal switch procedure involves removing a large part of the stomach. The small valve that allows the food to be released to the small intestine is left, along with the first part of the small intestine, known as the duodenum.
The middle section of the intestine is closed off and the last part is attached to the duodenum creating a duodenal switch.
The separated section of the intestine isn’t removed from the body like with the gastric sleeve. It is reattached to the end of the intestine. This allows bile and pancreatic digestive juices to travel to this piece of the intestine thus becoming the biliopancreatic diversion.
Once the procedure is complete and the food is digested, food will bypass most of the small intestine. This limits the absorption of calories and nutrients. Limiting the absorption of calories and nutrients and having a smaller size of the stomach leads to weight loss.
This is a lot of information and it is best a medical professional decides what type of surgery is best for you? Are you wondering which surgery is best for you? Find out by answering a few questions below:
This entry was posted in Uncategorized. Bookmark the permalink.